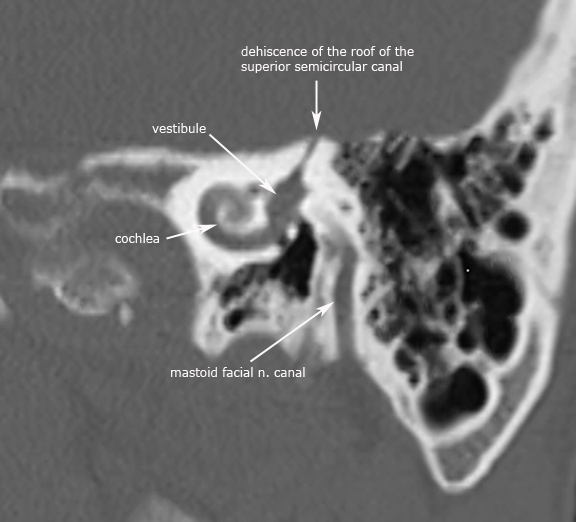
→The aetiopathogenesis of superior semicircular dehiscence (SCD) is a hypothesis that it is a developmental or congenital.Usually developmental defect should be symptomatic from birth. One possible is SCD why it presents first in adults life is that the dehiscent require a second insult to be symptomatic which causes the abnormally thin layer of bone overlying superior semicircular canal (SCC) to disrupt. e.g. head trauma.
Other number of different causes have been discussed such as erosion of the bone caused by neoplasm, inflammatory disease, arachnoid granulation or infectious reason but none of these could be verified as plausible.
Clinically it presents with:
- Vestibular symptoms induced by loud sounds or the manouevers such as coughing, sneezing, or staining.
- Auditory symptoms described as hyperacusis for bone conducted sounds. These patient may complain that they can hear, in the affected ear, their own eye movements or the impact of their feet during walking.
- Patient with SCD may develop nystagmus in response to loud sound (Tulio phenomenon).
- Many also develop nystagmus in response to the Valsalvaa maneuver or presence in the EAC (Hennebert sign). The ais of evoked nystagmus typically aligns the plane of dehiscent superior semicircular canal.
- Proportion of patients tilts their head in the plane of affected superiors SCC in responds to loud sounds.
Surgical Care
Surgical correction of superior canal dehiscence syndrome (SCDS) is reserved for patients with severe disabling symptoms.
Recently, albeit rare, it has been found that children also can have with superior canal dehiscence. They are almost always asymptomatic, and their management is no different from that of adults. Usually, they present with auditory complaints initially, and conservative management is recommended; however, if a child has complaints of vertigo, surgical management may be indicated.
The treatment options for patients with SCDS are still expanding, with new innovative methods under development.
Traditional middle fossa craniotomy and repair of fistula
In this procedure, patients undergo a middle cranial fossa craniotomy on the affected side. The temporal lobe is gently retracted. Upon elevation of the dura, care is required to avoid stretching the greater superficial petrosal nerve, which could injure the facial nerve. The region of the superior semicircular canal is located with identification of the arcuate eminence. A dehiscence of the superior semicircular canal can be covered with bone wax, bone cement, or fascia, or the canal can be ablated with wax or bone cement.
Endoscopic craniotomy approach
In this procedure, patients undergo a middle cranial fossa craniotomy through a small, limited-access craniotomy of 2 cm or less on the affected side. The temporal lobe is gently retracted. Upon elevation of the dura, a small endoscope is gently inserted, and the dehiscence is identified and resurfaced. This approach has an average hospital stay of 2 days and a smaller incision than the typical middle fossa approach originally described. Presented at the Virginia Society of Otolaryngology in 2010, Shaia and Peng discussed 10 patients who underwent this modified approached relief of preoperative symptoms of more than 90% with no adverse outcomes. One patient had continued vestibular complaints for 12 months after the procedure that eventually resolved. This approach allows the surgeon visualization of the dehiscence without the need for a larger craniotomy.
Transmastoid superior canal occlusion
In this approach, a mastoidectomy is performed and the superior semicircular canal is identified near the ossicular heads. The superior semicircular canal is then ablated with a combination of tissue and fascia. Brantberg et al performed a superior canal–plugging procedure via a transmastoid approach in 2 patients. Postoperatively, sound- and pressure-induced symptoms and nystagmus were resolved in response to offending stimuli. Although this approach can be effective, the risk of sensorineural hearing loss increases with this procedure because of limited exposure versus middle fossa craniotomy.
Minimally invasive approach via transcanal oval and round window reinforcement
The optimal surgical treatment of superior canal dehiscence syndrome has yet to be determined. Rather than directly addressing the dehiscent canal via a middle fossa craniotomy, an innovative approach first described by Kartush suggested that dampening the inner ear’s sensitivity by reinforcing the oval and round windows may alleviate symptoms in some patients.
The concept is to reduce the effects of a third window at the superior semicircular canal by reinforcing the other 2 natural windows. By dampening the presumed hyper compliance of the inner ear at the round windows, rather than intracranial, the risks of craniotomy, which include death, stroke, cranial palsies, and cerebrospinal fluid leaks, are avoided.
This procedure can be performed under local anesthesia. A transcanal approach to the middle ear is performed with elevation of the tympanic membrane. Small amounts of fascia are harvested from a postauricular incision are used to reinforce both the oval and round windows. The risks of the procedure, performed on an outpatient basis, are extremely low.
The preliminary study by Kartush in 2002 propagated discussions with others in the field of otology/neurology. As a result, a combined multi-institutional study under the direction of Silverstein was initiated in 2011 and was presented at the 2012 American Academy of Otolaryngology Annual meeting.
Twenty-two patients from 4 centers who opted for the minimally invasive approach via transcanal oval and/or round window reinforcement were studied. In this study, most had only round window reinforcement. Symptoms improved in nearly all patients treated with this novel method. A total of 21 patients completed a postoperative survey, grading preoperative and postoperative symptom severity. The questionnaire measured the 9 symptoms, including autophony, sensitivity to bone conduction, pulsatile tinnitus, sensitivity to loud sounds, dizziness on straining, dizziness on increased middle ear pressure loss, aural fullness, and imbalance. Analysis revealed statistically significant improvement in nearly all symptoms. The only symptom that did not improve was hearing loss.
If future studies confirm that such a minimally invasive procedure is routinely effective, middle fossa craniotomy or transmastoid approaches with resurfacing or occlusion of the canal could then be reserved for patients with persistent symptoms.
Combination approach
Gianoli and Soileau have advocated a combination approach. In this technique, the superior canal defect is repaired via the middle fossa approach with concomitant reinforcement of the oval and round windows. The authors claim improved outcomes over middle fossa repair alone, reporting a resolution of vertigo in 24 cases with a 5-year follow-up period.